
Stroke rehabilitation plays a pivotal role in restoring functional independence and improving quality of life in patients who sober neurological deficits following intracerebral haemorrhage. The thalamus, a key relay centre in the brain, when aBected by haemorrhage, can lead to significant motor, sensory, and cognitive impairments. Early and structured rehabilitation is essential to maximize recovery potential. This case report presents a 54-year-old hypertensive male who suBered a right thalamic bleed, resulting in left-sided hemiparesis and speech disturbances. Emphasis is placed on his rehabilitation journey—starting from bedside physiotherapy to intensive inpatient rehabilitation—demonstrating the critical impact of multidisciplinary therapy on his functional outcomes.
A 54-year-old male from Chhattisgarh, with known comorbidities of Hypertension, was apparently well until 23rd July 2024, when he developed sudden onset weakness of left upper limb and lower limb, speech disturbances, reduced consciousness. He was taken to nearby hospital and radio imaging was done – found to have right thalamic bleed. He was managed conservatively. He was started on bedside physiotherapy and was later referred to CMC Vellore for rehabilitation. Rehabilitation was initiated and he achieved independent sitting and required maximum assistance for standing. For further rehabilitation he was admitted in HCAH Bangalore.
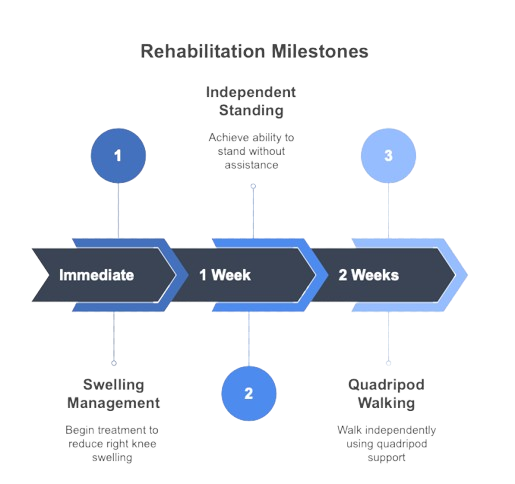
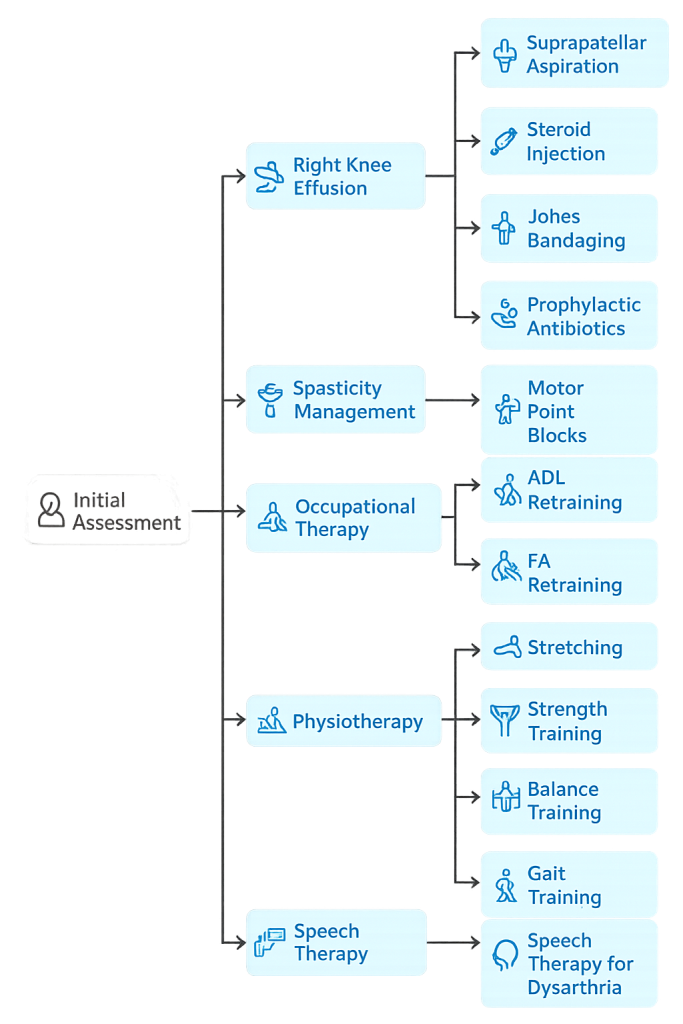

At the time of discharge, he was hemodynamically stable, was able to sit and stand independently. He was independent for activities of daily living. Significant reduction in Knee swelling & pain was n oted and he was a ble to walk with Q uadri pod support.
This case highlights the importance of early, structured, and multidisciplinary rehabilitation in improving functional outcomes following a thalamic haemorrhage. Structured Evaluation and neurorehabilitation interventions by PMR, played a key role in enhancing mobility and independence in daily activities for the patient. Continued rehabilitation support remains essential for maximizing long-term recovery and quality of life.


