
Sleep disturbances are highly prevalent in patients with advanced illness, affecting up to 60–80% of individuals in palliative care settings. Insomnia, fragmented sleep, and daytime fatigue can significantly impair physical comfort, emotional well-being, and overall quality of life. These disturbances are often multifactorial, arising from pain, medications, psychological distress, environmental factors, and disease progression.
In advanced illness, poor sleep not only worsens fatigue but also amplifies symptoms such as pain, anxiety, depression, and cognitive dysfunction, creating a distressing cycle. Therefore, addressing sleep disturbances becomes an essential component of holistic palliative care.
Sleep hygiene refers to a set of behavioral and environmental practices that promote better sleep quality. In the context of advanced illness, a gentle, individualized approach is required—focusing on comfort, practicality, and patient preferences rather than rigid rules.
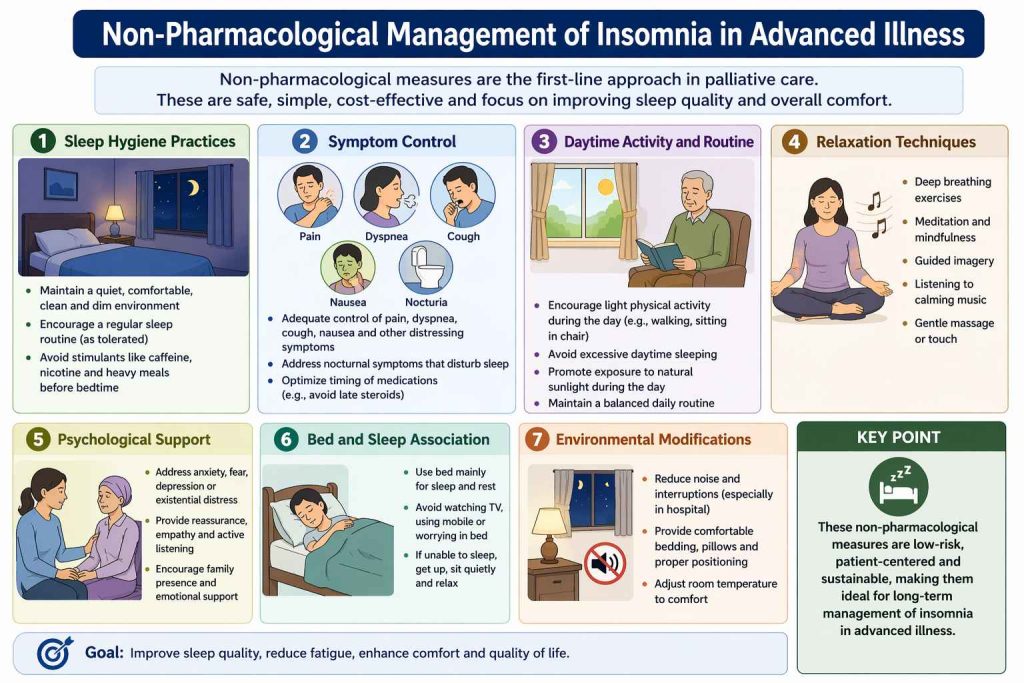
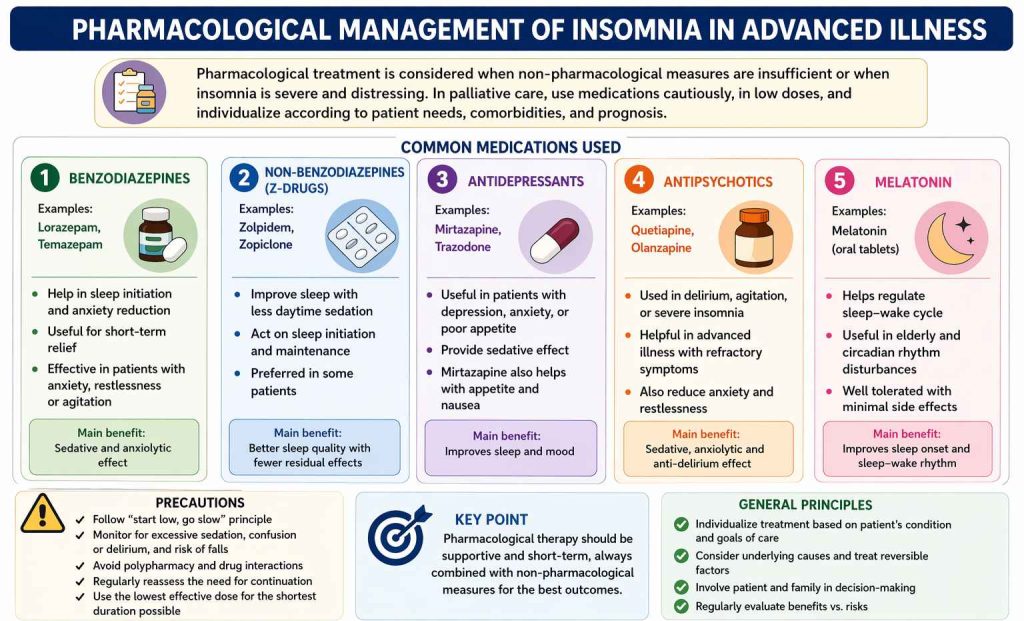
Management of insomnia in advanced illness requires a holistic and stepwise approach, focusing on identifying and addressing reversible causes while ensuring patient comfort. Since sleep disturbances are often multifactorial, treatment should begin with assessment of physical, psychological, and environmental factors contributing to poor sleep. In palliative care, the emphasis is on simple, low-burden interventions, with non-pharmacological measures forming the cornerstone of management. Pharmacological therapy is reserved for patients with persistent or severe symptoms.


I am a physician specialized in Palliative Medicine (MD) with a strong commitment to improving the quality of life for patients with life-limiting illnesses. My clinical focus is on comprehensive symptom management, holistic patient care, and psychosocial support for patients and families.Beyond clinical practice, I am deeply interested in palliative care education, research, and integrating evidence-based practices into patient-centered care. I aim to contribute to the growth of palliative care services, raise awareness about end-of-life issues, and advocate for a more compassionate healthcare system.