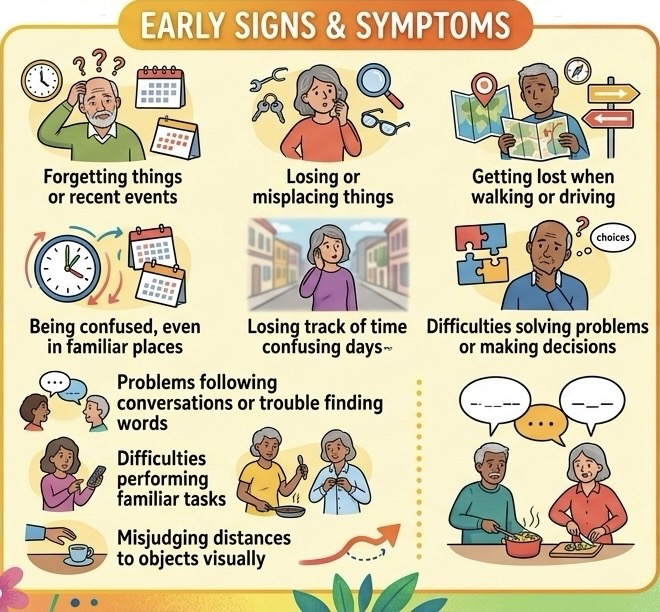
Palliative Care for Advanced Dementia
- Dementia is a progressive neurodegenerative syndrome characterised by a decline in cognitive functions such as memory, language, thinking, and the ability to perform daily activities. As the condition worsens, patients have more functional dependence, altered behaviour, and difficulty swallowing and communicating. When dementia reaches an advanced stage, it can be fatal and is linked to complications like infections, eating disorders, and a high death rate.
- Dementia is a worldwide health issue, especially for the elderly. Over 55 million people worldwide have been identified to have dementia, and as the world’s population ages, this figure is predicted to rise substantially. Alzheimer’s disease is the most common cause of dementia, accounting for 60–70% of cases. Dementia affects 5–8% of people over 60, and its prevalence rises noticeably with age.
Common risk factors for developing dementia
- age (more common in those 65 or older)
- high blood pressure
- high blood sugar
- being overweight
- smoking
- drinking too much alcohol
- being physically inactive
- being socially isolated
- depression
Issues in Dementia
- Cognitive impairment – progressive decline in memory, thinking, judgment, and orientation.
- Communication difficulties – inability to express needs, pain, or discomfort effectively.
- Behavioral and psychological symptoms – agitation, aggression, depression, anxiety, hallucinations, and sleep disturbances.
- Functional dependence – progressive loss of ability to perform activities of daily living such as bathing, dressing, and eating.
- Swallowing difficulties (dysphagia)
- Recurrent infections
- Malnutrition
- Pain
- Pressure ulcers
- Caregiver burden and emotional stress affecting family members and caregivers.
Symptom-wise Palliative Management in Dementia
1.Pain
Symptoms: facial grimacing, agitation, restlessness, withdrawal, reduced mobility.
Palliative Management
- Regular pain assessment using observational tools (e.g., PAINAD scale).
- First-line analgesics such as paracetamol.
- Opioids (e.g., morphine) for moderate to severe pain.
- Treat underlying causes such as arthritis, fractures, or pressure ulcers.
- Non-pharmacological approaches including massage, repositioning, and comfort measures.
2.Agitation and Behavioural Symptoms
Symptoms: restlessness, aggression, wandering, sleep disturbance.
Palliative Management
- Identify triggers such as pain, infection, or environmental stress.
- Non-pharmacological interventions:
- Calm environment
-
- Familiar caregivers
-
- Music therapy or reassurance
-
- If severe: cautious use of medications such as antipsychotics or sedatives
- In refractory cases at end of life, palliative sedation may be considered.
3.Dyspnea (Breathlessness)
Symptoms: labored breathing, anxiety, air hunger.
Palliative Management
- Treat reversible causes (infection, aspiration).
- Oxygen therapy if hypoxic.
- Low-dose opioids to relieve breathlessness.
- Positioning and calm reassurance to reduce anxiety.
4.Dysphagia and Feeding Problems
Symptoms: choking, aspiration, poor oral intake, weight loss.
Palliative Management
- Careful hand feeding with modified food textures.
- Thickened liquids and upright feeding position.
- Focus on comfort feeding rather than aggressive artificial nutrition.
- Educate families about the risks and benefits of feeding tubes.
5.Infections (eg: Pneumonia, UTI)
Symptoms: fever, cough, confusion, functional decline.
Palliative Management
- Symptom-focused treatment such as antipyretics, hydration, and antibiotics when appropriate.
- Discuss goals of care regarding hospitalization or aggressive treatment.
- Emphasis on comfort and quality of life.
6.Pressure Ulcers and Immobility
Symptoms: skin breakdown, pain, infection.
Palliative Management
- Frequent repositioning and pressure-relieving mattresses.
- Proper skin care and hygiene.
- Wound care and analgesia for pain relief.
7.Cognitive Impairment
Cognitive impairment in advanced dementia leads to progressive memory loss, confusion, poor judgment, and difficulty performing daily activities. The palliative approach focuses on maintaining function, ensuring safety, and improving quality of life rather than reversing the decline.
Palliative management includes
A) Non-pharmacological approach
- Provide a structured and familiar environment to reduce confusion.
- Use orientation cues such as clocks, calendars, and family photographs.
- Encourage simple daily routines and familiar activities.
- Use clear, simple communication and give one instruction at a time.
- Ensure adequate sleep, nutrition, and hydration.
- Promote social interaction and caregiver support.
B)Pharmacological approach
- Cholinesterase inhibitors (donepezil, rivastigmine, galantamine) may slow cognitive decline in earlier stages.
- Memantine may be used in moderate to severe dementia to improve cognition and daily functioning.
8.Psychological and Emotional Distress
Symptoms: anxiety, depression, fear.
Palliative Management
- Emotional reassurance and familiar surroundings.
- Support from family and caregivers.
- Counseling and spiritual care when needed.
Advance care planning:
Patients can express their preferences for future medical care through advance care planning (ACP), which is based on patient autonomy. End-of-life decisions must be made by family members or designated surrogates as dementia patients gradually lose their capacity to make decisions. To lessen the emotional strain on families and prevent unwelcome medical interventions, early conversations about prognosis, treatment preferences, and advance directives are crucial. In more advanced stages, doctors may also need to evaluate a patient’s capacity for making decisions, which encompasses comprehension of information, situational awareness, reasoning about treatment options, and communication of a decision.
Conclusion:
Palliative care plays a crucial role in the management of advanced dementia by focusing on symptom relief, comfort, and quality of life. As dementia progresses and patients lose decision-making capacity, a palliative approach helps address physical symptoms, psychological distress, and caregiver burden. Early integration of palliative care ensures compassionate, patient-centered care while supporting families and maintaining dignity in the final stages of the disease.