
Lymphedema is a chronic condition characterised by the accumulation of protein-rich lymphatic fluid in the interstitial tissues, resulting from impaired lymphatic drainage. This leads to persistent swelling, most commonly affecting the limbs, and may be associated with heaviness, discomfort, skin changes, and reduced mobility.
Lymphedema can be classified as primary (due to congenital or developmental abnormalities of the lymphatic system) or secondary, which is more common and occurs due to damage or obstruction of lymphatic vessels. In cancer patients, secondary lymphedema typically develops as a result of tumour infiltration, lymph node dissection, or radiation therapy.
In advanced cancer, the impact of lymphedema goes beyond physical symptoms. It can lead to pain, impaired function, skin changes, and psychological distress, significantly affecting quality of life. As patients approach later stages of illness, the goal of care shifts from aggressive interventions to comfort-focused, patient-centred management.
A gentle approach to lymphedema management prioritises symptom relief, simplicity, and patient comfort, avoiding burdensome treatments while maintaining dignity and quality of life.
Assessment – It should be start with complete clinical history.
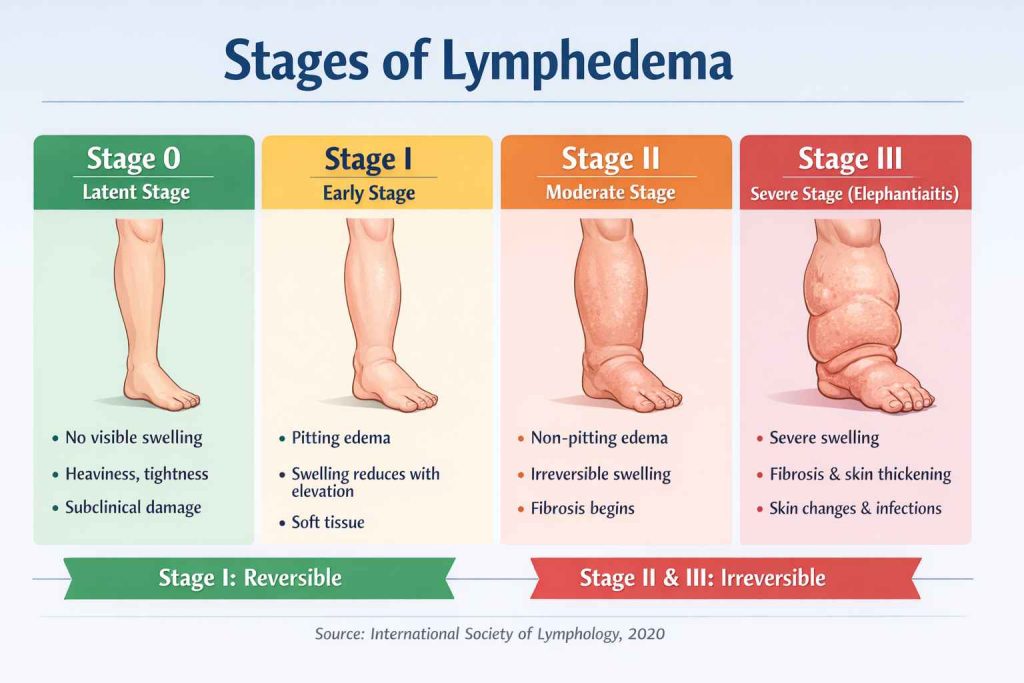
Site and extent of swelling
Skin changes (thickening, fibrosis, redness)
Presence of wounds or infection
Pitting vs. non-pitting edema.
Tissue consistency (soft, firm, fibrotic)
Temperature changes
In advanced cancer, measurements should be simple and non-burdensome.
Care in Lymphedema – Care in lymphedema focuses on reducing swelling, preventing complications, relieving discomfort, and maintaining function.
Skin care – Keep the skin clean and well moisturized to prevent dryness, cracks, and infection. Avoid cuts, burns, and insect bites. Avoid blood pressure measurement and Intravenous line in affected limb.
Limb elevation – Elevating the affected limb may help reduce swelling and improve comfort.
Compression therapy – Use compression bandages or garments if tolerated and appropriate. In advanced cancer, compression should be gentle and individualized.
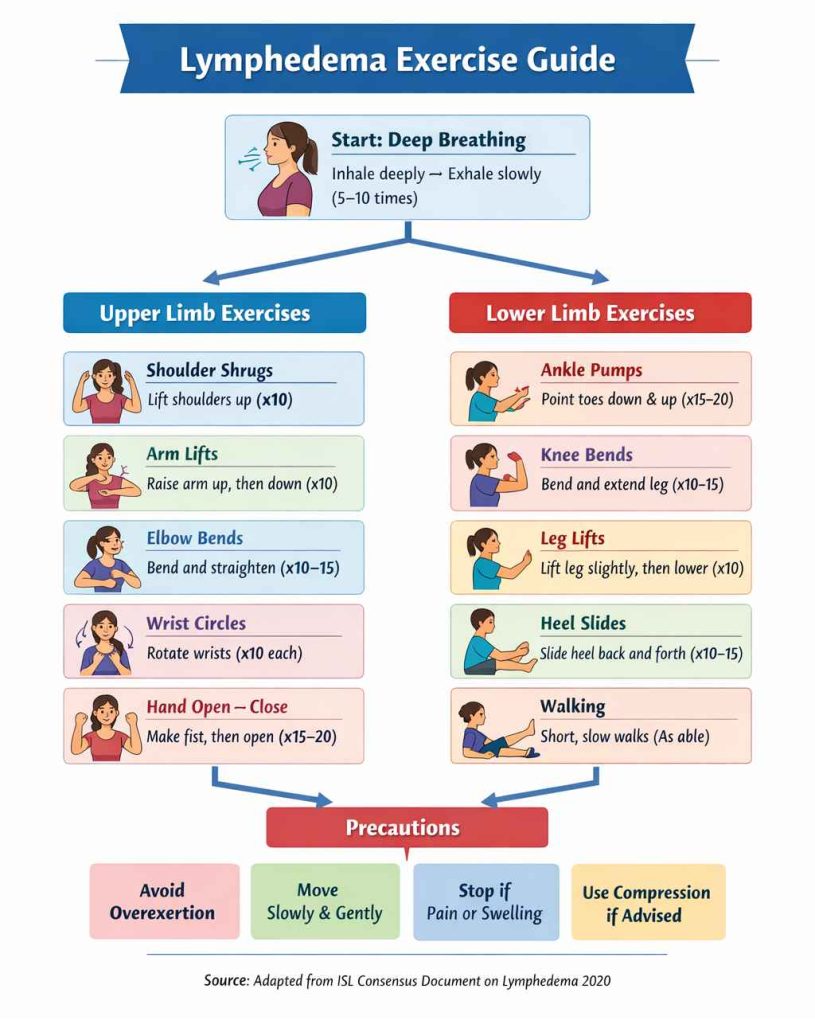
Exercise and movement – Encourage gentle range-of-motion exercises and light activity to improve lymph flow and maintain mobility.
Manual lymphatic drainage – Gentle lymphatic massage by a trained professional may help selected patients, especially when it improves comfort.
Infection prevention – Watch for redness, warmth, pain, or fever suggestive of cellulitis, and treat early.
Pain and symptom relief – Manage pain, heaviness, and discomfort with analgesics, positioning, and supportive care.
Psychological support – Lymphedema can affect body image and mood, so emotional support and reassurance are important.
Patient and caregiver education – Teach proper skin care, limb care, warning signs of infection and safe use of compression.
Complications due to Lymphedema – Lymphedema in advanced cancer can lead to several complications that significantly affect patient comfort and quality of life. Persistent swelling and impaired lymphatic drainage increase the risk of recurrent infections, particularly cellulitis. Skin changes such as thickening, dryness, and ulceration may occur, making the limb more vulnerable to injury. Over time, patients may develop reduced mobility, pain, and functional limitation, which can further contribute to dependency and emotional distress. In advanced stages, these complications require careful, gentle management to prevent worsening symptoms while maintaining patient dignity
Lymphedema in advanced cancer is a chronic and distressing condition that significantly impacts physical comfort, function, and quality of life. A gentle, palliative approach to management—focused on symptom relief, simple interventions, and patient preferences—is essential. By emphasizing skin care, light compression, gentle exercises, and early management of complications, healthcare providers can reduce discomfort while avoiding burdensome treatments. Integrating palliative care ensures holistic support, helping patients maintain comfort, dignity, and the best possible quality of life in the advanced stages of illness.

I am a physician specialized in Palliative Medicine (MD) with a strong commitment to improving the quality of life for patients with life-limiting illnesses. My clinical focus is on comprehensive symptom management, holistic patient care, and psychosocial support for patients and families.Beyond clinical practice, I am deeply interested in palliative care education, research, and integrating evidence-based practices into patient-centered care. I aim to contribute to the growth of palliative care services, raise awareness about end-of-life issues, and advocate for a more compassionate healthcare system.