
End-of-life care has become an increasingly important aspect of modern medicine, especially with advances in life-sustaining technologies that can prolong survival even in irreversible and terminal conditions. While these interventions can be life-saving in many situations, they may also lead to prolonged suffering, loss of dignity, and a reduced quality of life when recovery is no longer possible. This has led to growing discussions around the concept of a “good death”, where care focuses not on prolonging life at all costs, but on ensuring comfort, dignity, and respect for patient wishes.
In this context, passive euthanasia has emerged as a significant ethical and legal consideration. It involves the withdrawal or withholding of life-sustaining treatment in patients with terminal or irreversible illness, allowing the natural process of death to occur. In India, the recognition of passive euthanasia by the Supreme Court, particularly through landmark judgments, reflects an evolving understanding of the patient’s right to die with dignity.
The Harish Rana case has brought renewed attention to these issues by highlighting the real-world challenges faced by patients, families, and healthcare professionals in making end-of-life decisions. It underscores the emotional, ethical, and legal complexities involved when continuing treatment may no longer be beneficial. The case also emphasises the importance of advance care planning, clear communication, and palliative care integration in ensuring that decisions are aligned with the patient’s values and best interests.
By examining this case, we gain insight into how legal frameworks and clinical practice intersect, and why it is essential to develop compassionate, patient-centred approaches to end-of-life care in India.
The term “passive euthanasia” is increasingly considered misleading in modern palliative and end-of-life care discussions. Traditionally, euthanasia refers to the intentional act of ending a person’s life to relieve suffering, usually through a direct intervention intended to cause death. In contrast, withholding or withdrawing life-sustaining treatment does not aim to cause death, but rather recognizes that further medical treatment is futile or burdensome and allows the underlying disease to take its natural course.
Many clinicians, ethicists, and palliative care specialists therefore prefer terms such as “withholding or withdrawal of life-sustaining treatment,” “allowing natural death,” or “end-of-life decision-making” instead of passive euthanasia. The primary intention in these situations is to respect patient autonomy, reduce suffering, and avoid disproportionate medical interventions, rather than intentionally ending life.
In the Indian legal context, however, the phrase “passive euthanasia” continues to be used in Supreme Court judgments and public discussions. Despite this terminology, the practice legally refers to withdrawal or withholding of futile treatment under defined safeguards and should be clearly distinguished from euthanasia involving intentional life-ending actions.
Euthanasia refers to the intentional act of ending a person’s life to relieve suffering, usually in patients with severe, incurable, or terminal illnesses. It is considered in situations where a patient experiences unbearable pain, loss of dignity, or poor quality of life with no reasonable chance of recovery.
The Harish Rana case involved a patient suffering from a severe, irreversible neurological condition, where he was dependent on life-sustaining treatment with minimal chances of recovery. Due to the prolonged illness and poor prognosis, the family approached the court seeking permission for withdrawal of life support, highlighting the patient’s suffering and lack of meaningful quality of life. The case brought forward the practical challenges of implementing passive euthanasia in India, including medical evaluation, legal procedures, and ethical decision-making.
It became significant as it demonstrated how the principles laid down in the Common Cause (2018) judgment are applied in real clinical situations, especially in the absence of clear advance directives. The case also emphasized the emotional burden on families and the critical role of healthcare professionals in guiding end-of-life decisions.
Implementing passive euthanasia in India presents multiple challenges at the intersection of medical practice, law, and ethics. Despite legal recognition, the process can be complex and emotionally demanding for both families and healthcare professionals. Families often face significant psychological stress while making end-of-life decisions, especially in the absence of clear advance directives. Healthcare providers may also experience ethical dilemmas and fear of legal consequences, which can delay decision-making. Additionally, lack of awareness about legal provisions, cultural and religious beliefs surrounding death, and limited access to palliative care services further complicate the process. Ensuring proper documentation, coordination between medical boards, and adherence to legal safeguards can also be time-consuming and difficult in real-world settings.
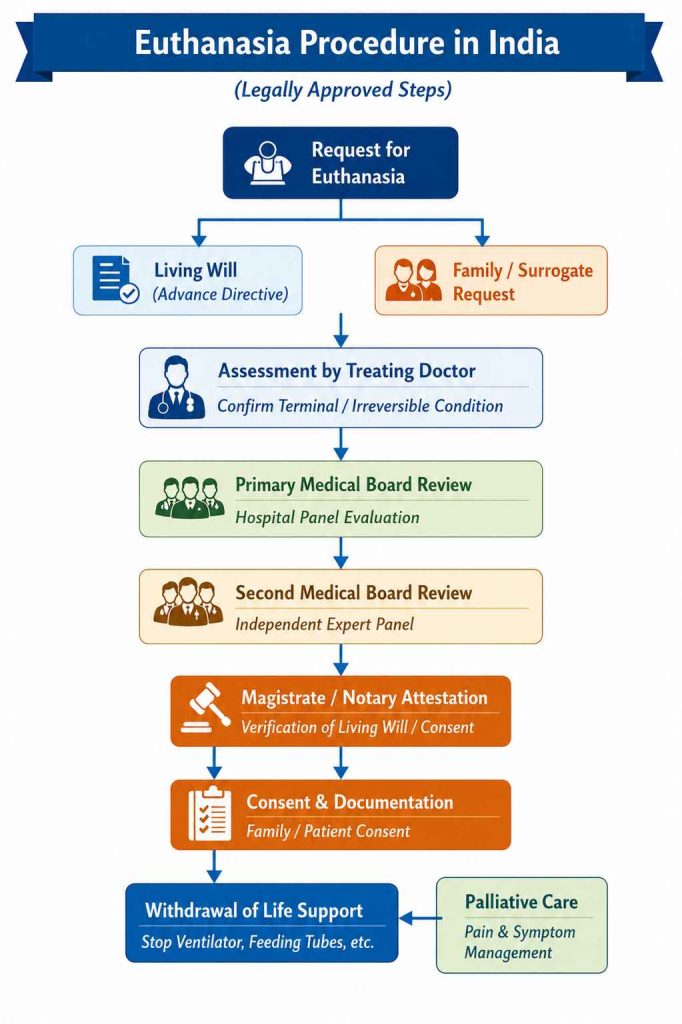
Euthanasia represents an important evolution in end-of-life care, balancing medical ethics, legal safeguards, and patient autonomy. In India, landmark judgments have recognized the right to die with dignity, allowing withdrawal of futile life-sustaining treatment under strict guidelines. However, its practical implementation remains challenging due to emotional, ethical, and systemic factors. Strengthening awareness, simplifying procedures, and integrating palliative care into routine practice are essential to ensure that patients receive compassionate, dignified, and patient-centered care at the end of life.

I am a physician specialized in Palliative Medicine (MD) with a strong commitment to improving the quality of life for patients with life-limiting illnesses. My clinical focus is on comprehensive symptom management, holistic patient care, and psychosocial support for patients and families.Beyond clinical practice, I am deeply interested in palliative care education, research, and integrating evidence-based practices into patient-centered care. I aim to contribute to the growth of palliative care services, raise awareness about end-of-life issues, and advocate for a more compassionate healthcare system.